Nat Med: Wang Zhang, Lin Lifeng, Guan Weijie and Sun Jiufeng Reveal that Environmental Exposure Affects Respiratory Health Outcomes through Airway Microbiota Disorder
2023-06-243450On June 22, 2023, the team led by Wang Zhang with South China Normal University, the team led by Lin Lifeng and Sun Jiufeng with Guangdong Provincial Center for Disease Control and Prevention, the team led by Guan Weijie with the First Affiliated Hospital of Guangzhou Medical University, Guangzhou Research Institute of Respiratory Health and the State Key Laboratory of Respiratory Disease published a research article entitled “The airway microbiome mediates the interaction between environmental exposure and respiratory health in humans” in the journal of Nature Medicine. Through multi-omics analysis of airway microbiome among large populations, it revealed the relationship between environmental exposure, airway microbiome and respiratory health (Figure 1).

Based on the an epidemiological survey project of chronic obstructive pulmonary disease (COPD) residents in Guangdong Province in 2019, the study conducted questionnaire survey, lung function examination, body measurement and collected the induced sputum among 3,800 residents in 36 neighborhood committees in 18 communities of 6 cities / regions,. After strict quality control, induced sputum was subjected to bacterial 16S rRNA amplicon (n=1,651), fungal ITS amplicon (n=719), and metagenomic (n=1,128) sequencing. First, the study established the two-way mediating effect model of pollution exposure (smoking, secondhand smoking, air pollution, biofuel exposure, occupational exposure), airway microbiota (functional modules of bacteria, fungi and metagenomic, antibiotic resistance genes, bacterial virulence factor), respiratory health outcomes (lung function, respiratory symptoms score), and found that airway microbiota had a significant mediation effect in environmental exposure and respiratory health outcomes. Meanwhile, different pollution exposure factors acted through the mediation of different bacterial or fungal communities. Smoking mainly affected bacterial communities, and atmospheric fine particulate matter (PM2.5) mainly affected fungal communities. A further interactive statistical model analysis revealed significant interactions between airway microbiome, occupational contamination exposure and respiratory symptom score. Among them, the associations between respiratory symptom scores and occupational pollution exposure were significant different between two subgroups divided by Neisseria taxa. Compared to the Neisseria-low subgroup, Neisseria-high subgroup was associated with a 2.25-fold increased risk of high respiratory symptom burden in association with occupational pollution, which may act through the increased abundance of Aspergillus in the fungal flora. The results suggested that the risk stratification and assessment of environmental exposure may be based on airway microbiota.
Based on the characteristics of respiratory bacterial and fungal flora, the individualized airway microbiome health index (AMHI) was measured. It was found that AMHI changed simultaneously with pollution exposure, respiratory symptoms and respiratory diseases, suggesting that the index may indicate the potential respiratory health risk caused by individual pollution exposure. Applied to the global public airway microbiota data, it was found that AMHI showed a similar declining trend in patients compared with the healthy population with different public libraries, indicating that the index was universal to a certain extent. Environmental exposure is an important risk factor for the early onset of COPD. Through multiple network analysis, the study found that environmental exposure can promote the “bacteria-fungi” interaction at the airway. The interaction pattern was significantly enhanced from healthy population, COPD risk population, to patients with COPD, and the bacterial drivers of such interaction significantly contributed to the flora function changes from healthy population to COPD. Individualized health index and interaction networks based on respiratory bacteria and fungi may provide potential novel identifiers for early onset of COPD.
In conclusion, this study has revealed the possible way that environmental exposure affects respiratory health through a large-scale population’s airway microbiome analysis. The exposure–airway microbiome–health outcome interactions may help identify microbial risk factors underlying the effect of exposures on respiratory health. Airway microbiome may affect the individual health effect with environmental exposure, which provides a scientific evidence for the microbiome-based environmental risk stratification and the interventions targeting the microbiome for risk prevention.
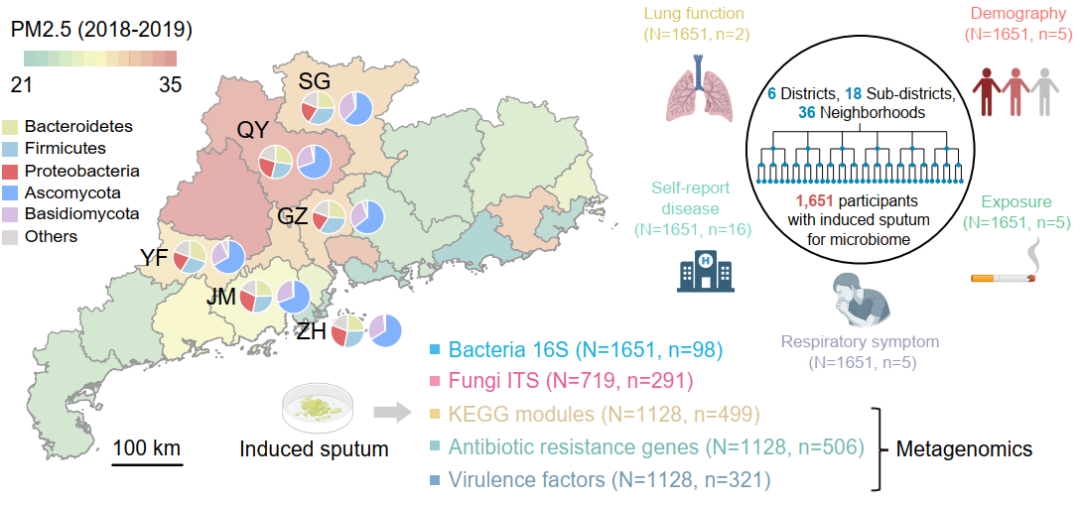
Figure 1. Main design and technical route of this study
Original link:https://doi.org/10.1038/s41591-023-02424-2
















